Thyroid Eye Disease & Treatment
I. Introduction
One of the most common problems people have with thyroid gland disease is varying degrees of eye difficulty. Eye problems are usually caused by abnormal swelling of the soft tissue surrounding the eyes and by enlargement of the muscles that move the eyes and open the eyelids.
The reason for the swelling is an autoimmune reaction. The term “autoimmune” means that the immune system in your body attacks a part of your body, in this case the soft tissues of the eye. It is the same autoimmune process that causes the thyroid gland to be abnormal (usually hyperactive). The thyroid gland problem and the eye problem are usually separated by years.
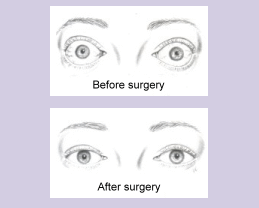
As a result of the swelling, the eyes may protrude forward; there may be retraction of the upper eyelids which forces the lids to part; there is an inability to fully close the eyelids, and a large portion of the eyeball is exposed. This leads to prominent eyes, a fixed staring expression, and eyes that dry out constantly. (See figure 5).
II. Onset of symptoms
Some patients start with these symptoms as soon as the thyroid gland becomes hyperactive (or in some instances, hypoactive). In most cases, the eye changes develop slowly, years after the abnormal thyroid gland activity commences.
There can be pressure on the eyes, excessive tearing and double vision. It usually affects both eyes but can be unilateral, especially early in its course.
Overexposure of the eyes and inability to completely close the eyes at night can result in drying of the cornea. Dryness of the cornea can cause considerable discomfort and visual problems such as blurred vision, foreign body sensation or light sensitivity.
As the muscles slowly enlarge, movement of the eyes may become restricted. This restriction may cause misalignment of the two eyes, resulting in double vision.
If the swelling is severe, the high intraorbital pressure can cause compression of the optic nerve. If this happens, a person can experience a slow loss of vision and even blindness if the condition is not corrected.
III. Nonsurgical treatment
If the thyroid gland is hyperactive, it can be treated which may sometimes relieve the associated eye problems. This is rare in that most cases of thyroid eye problems occur many years after (or sometimes before) the actual gland problems.
Sleeping with the head elevated and using diuretics can reduce swelling. Topical ointments and artificial tears can lubricate the eye and prevent the surface from drying out. At bedtime it is sometimes necessary to tape the eyes closed or use plastic shields if the eyes cannot close during sleep. Tinted glasses with side guards are sometimes necessary. In conjunction with an endocrinologist, steroid pills or medications stronger than steroids such as immunosuppressive agents may be used. Sometimes even radiation therapy is used. This decision is usually made by the endocrinologist in conjunction with the radiation specialist and the oculoplastic surgeon.
IV. Surgical treatment
In most severe cases, surgery is sometimes necessary to improve the condition. The function and appearance of the eyes can usually be improved with eyelid and/or orbital surgery. The corrective procedures are staged and will depend on the severity of the eye problems as to which stage is done first.
Orbital decompression (removal of part of the bony orbit to relieve pressure within the eye socket) can prevent damage to the optic nerve. It also allows the eyes to move back into a more normal position within the sockets.
Eye muscle surgery is done after the decompression (if it is necessary). The enlarged muscles that control eye movement are repositioned to properly align the eyes and correct the double vision.
Removal of excess orbital fat in the eyelids can improve the patient’s appearance. Eyelid surgical procedures to adjust the position of the eyelids usually help minimize retraction of the lids.
V. Summary
Dr. Carey has medically and surgically managed patients with thyroid eye disease for many years. He has a very large thyroid eye disease practice and is considered one of the leaders in the State in the management of ophthalmic problems of this difficult condition.
